What to Do When a Person with Dementia Wanders: Safety Guide for Caregivers
Worried about wandering in dementia? Discover why it happens, gentle prevention strategies, emergency steps, and caregiver support to keep your loved one safe without restricting dignity. Practical guide from KraftWald.
RESTLESSNESS & NEEDS
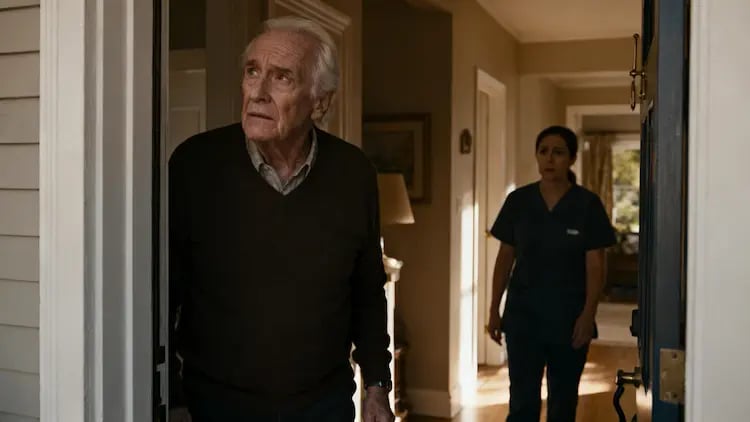
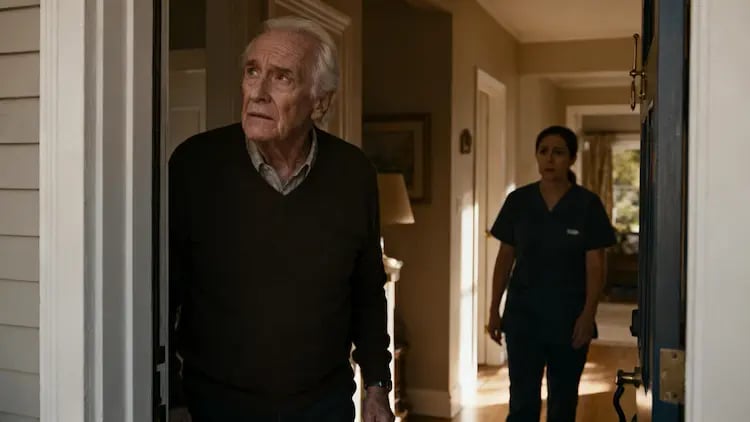
What to Do When Someone with Dementia Wanders Away
Post 23
A Gentle Guide to Safety, Orientation, and Dignity
The world of a person with dementia can shift suddenly.
Familiar rooms feel foreign.
Home stops feeling like home.
Sometimes the urge “I have to go” grows so strong that the door opens—and they leave.
For family caregivers, this can be one of the most frightening moments imaginable.
Panic. Guilt. Helplessness.
Many wonder:
“Haven’t I watched closely enough?”
🌿
The most important answer first: No.
Wandering is not your failure. It is a symptom of the disease.
This article offers calm guidance for moments of fear—before, during, and after wandering occurs. It helps you understand why it happens, how to respond in emergencies, and how to build everyday safety without sacrificing dignity or freedom.
(For background on dementia itself, see 👉 Post 6: Understanding Dementia – Causes, Types, and Symptoms.)
Why the Urge to Wander Arises
Wandering rarely means escape.
More often, it comes from a deep, wordless longing:
“I want to go home.”
“I need to go to work.”
“I have to leave.”
Even when someone is physically at home, the space may no longer feel familiar. The brain reaches for memories from earlier life—places of safety, purpose, and belonging. Today’s home can feel like a waiting room, while the real “home” lives somewhere in the past.
Other common triggers include:
Inner restlessness or need for movement — the body still craves purpose and rhythm. 👉 Post 2: From Restlessness to Calm – Meaningful Hand Activities
Boredom or under-stimulation — an empty day invites action.
Sensory overload — too much noise, light, or social input.
Old habits — decades of leaving for work at the same hour.
Diffuse anxiety — a vague but powerful sense that “something isn’t right.” 👉 Post 14: Emotions in Dementia – Understanding Fear, Grief, and Joy
🌱
These impulses are strong and often impossible to put into words. They are not stubbornness or defiance.
They are the disease speaking through movement.
Gentle Ways to Understand and Redirect the Urge
There is no perfect fix—but gentle strategies can guide the impulse safely.
Observe patterns
Notice when restlessness peaks.
After meals? Late afternoon? After visitors? During quiet moments?
Patterns help you anticipate and prepare.
Build in purposeful movement
Offer the body safe outlets:
daily walks, garden loops, folding laundry, sweeping leaves—small tasks with meaning. 👉 Post 3: Movement in Dementia – When the Body Remembers
Offer validating alternatives
Instead of correcting (“You’re already home”), try acknowledging the feeling:
“Yes, let’s go out together for a bit. Fresh air feels good.”
You join the impulse rather than fighting it—and often, the urge softens once movement begins.
Lean on familiar rituals
Repetition anchors the day:
afternoon coffee, a familiar song before dinner, hanging the coat in the same place. 👉 Post 1: Why Familiarity Matters So Much in Dementia
🌿
The goal is not to eliminate the urge—but to channel it gently and safely.
Creating Safety – Without Confinement
Safety does not have to mean restriction.
Think instead:
Safety = orientation + calm + small, dignified adjustments
An important legal note
In Germany, Austria, and Switzerland, locking doors or restricting freedom without court or guardianship approval is generally not permitted (freedom-restricting measures under Betreuungsrecht). In most cases, gentle environmental changes and supportive strategies are both lawful and sufficient.
Across the EU, call 112 in emergencies.
(If you live outside the EU, check your local emergency number and care regulations.)
Gently adapt the environment
Make the front door less visually prominent (curtain, shelf, or poster).
Store shoes, jackets, and keys out of sight—fewer cues mean fewer impulses.
Add a soft bell or wind chime to the door—a gentle alert for you, not a harsh alarm.
Use clear, simple signs: “Bathroom,” “Kitchen,” “Bedroom.” 👉 Post 8: Creating Gentle Transitions in Dementia
Install soft night lights—shadows and darkness can trigger fear.
Plan intentional movement
Same-time daily walks on familiar routes.
Indoor walking loops or protected garden paths in bad weather.
Meaningful activities like folding, swaying to music, or sorting items. 👉 Post 4: Creative Activities in Dementia – 5 Simple Ideas
Supportive Technology (Used Respectfully)
GPS wearables can provide peace of mind by alerting you if a boundary is crossed. Many include SOS buttons and fall detection.
When choosing a device, look for:
discreet, non-childish design
waterproof and durable
long battery life
simple app alerts
Widely used options in the EU include devices such as AngelSense or EU-focused providers like Invoxia / TechSilver.
Local dementia organizations or services often recommend region-specific options (for example, Otiom in Nordic and EU markets for its month-long battery life).
Technology should always support connection, not replace it—and ideally be used with consent or guardian agreement whenever possible.
If the Person Has Already Wandered
First: pause and breathe.
Your calm is one of the most effective tools you have.
Immediate steps checklist
Search nearby right away—garden, street, neighbors (people are often close).
Check familiar places: former home, church, park, café, cemetery, bus stop.
Alert neighbors and family quickly.
Call emergency services early:
Germany: 110
Austria: 133
Switzerland: 117
EU-wide: 112
Say: “A vulnerable person with dementia is missing.”
Prepare a recent photo, clothing description, and likely destinations.
Use GPS tracking if available.
When they return
No blame or scolding. They were not rejecting you—they were searching for safety.
Offer calm reassurance. They may be frightened or confused too.
Reflect gently later on possible triggers: Was it hunger, fatigue, noise, or overstimulation?
If wandering is new or escalating, consider a medical review. 👉 Post 6: Understanding Dementia
Rule Out Treatable Physical Causes
Restlessness can sometimes be eased when physical issues are addressed:
unmanaged pain
urinary tract infections
constipation
medication side effects
poor or fragmented sleep
A medical check can make a meaningful difference.
Spot Early Warning Signs
Wandering often announces itself quietly:
pacing or repetitive walking
repeated door checks
packing bags or personal items
frequent statements like “I have to go”
evening agitation (sundowning) 👉 Post 19: Sundowning – When Evenings Feel Heavy
Recognizing these early allows you to respond with movement, closeness, or calming activity before the urge escalates.
Caring for Yourself – The Emotional Load
Wandering is exhausting.
The vigilance. The fear. The guilt. The constant readiness.
These reactions are human—and common.
You carry so much, often without witnesses.
If you feel depleted, see:
👉 Post 13: Burnout in Family Caregivers
👉 Post 16: Anticipatory Grief – Missing Someone Still Here
👉 Post 20: When Care Steals Your Sleep
Your well-being matters too.
When to Seek Professional Support
Reach out if:
wandering increases
fear of injury grows
exhaustion becomes constant
Treatable factors—pain, depression, infection, medication effects, sleep issues—can improve quality of life. 👉 Post 18: Sleep Problems in Dementia
A GP, neurologist, or memory clinic can help you assess next steps.
Frequently Asked Questions
Why do they say “I want to go home” when we are already home?
“Home” often means safety and belonging from the past—not the current address.
Can wandering be fully prevented?
Not always, but routines, movement, and familiarity reduce it significantly. 👉 Post 8: Creating Gentle Transitions in Dementia
Are GPS trackers ethical?
Yes—when used respectfully for safety, and with consent if possible.
Does wandering mean late-stage dementia?
No. It can occur at any stage. 👉 Post 6: Understanding Dementia
🌟 Closing Thought
Wandering is painful—but it is also communication.
Each step expresses a need: for safety, familiarity, orientation.
When you understand instead of correct 👉 Post 9: Communication in Dementia – With Heart, Not Facts,
accompany instead of control,
and make small, thoughtful changes—
you create safety that holds gently, without confining.
Your presence brings calm and dignity, even when memories fade.
You are doing an extraordinary amount.
You do not walk this path alone.
🔗 Further Reading
👉 Post 1: Why Familiarity Matters So Much in Dementia
👉 Post 2: From Restlessness to Calm – Meaningful Hand Activities
👉 Post 3: Movement in Dementia – When the Body Remembers
👉 Post 13: Burnout in Family Caregivers
👉 Post 14: Emotions in Dementia – Understanding Fear, Grief, and Joy
👉 Post 19: Sundowning – When Evenings Feel Heavy
👉 Post 20: When Care Steals Your Sleep
👉 Next: Post 24 –
👈 Previous: Post 22: 7 Dementia-Friendly Everyday Recipes